The Low-FODMAP Diet: A Clinical Protocol for Managing IBS and SIBO
Understanding the biochemistry of carbohydrate fermentation and how to identify your unique dietary triggers.
What Does FODMAP Actually Mean?
The term FODMAP is an acronym developed by researchers at Monash University to group together specific types of short-chain carbohydrates (sugars and fibers) that the human digestive system struggles to process. The acronym stands for:
- Fermentable: Carbohydrates that are easily broken down by bacteria in the gut, producing gas as a byproduct.
- Oligosaccharides: Fructans and GOS (found heavily in wheat, rye, onions, and garlic).
- Disaccharides: Lactose (found in dairy products like milk, yogurt, and soft cheeses).
- Monosaccharides: Fructose (found in honey, high-fructose corn syrup, and fruits like apples and pears).
- And Polyols: Sugar alcohols such as sorbitol and mannitol (found in some fruits/vegetables and often used as artificial sweeteners).
The Biochemistry of Digestive Distress
In a person with a perfectly functioning gut, eating high-FODMAP foods causes little to no issue. But for people with Irritable Bowel Syndrome (IBS) or Small Intestinal Bacterial Overgrowth (SIBO), these specific carbohydrates set off a cascade of severe physical distress.
The reason? These short-chain carbohydrates don't absorb well in the small intestine—they travel through relatively intact and land in the large intestine (colon). Once there, two things happen:
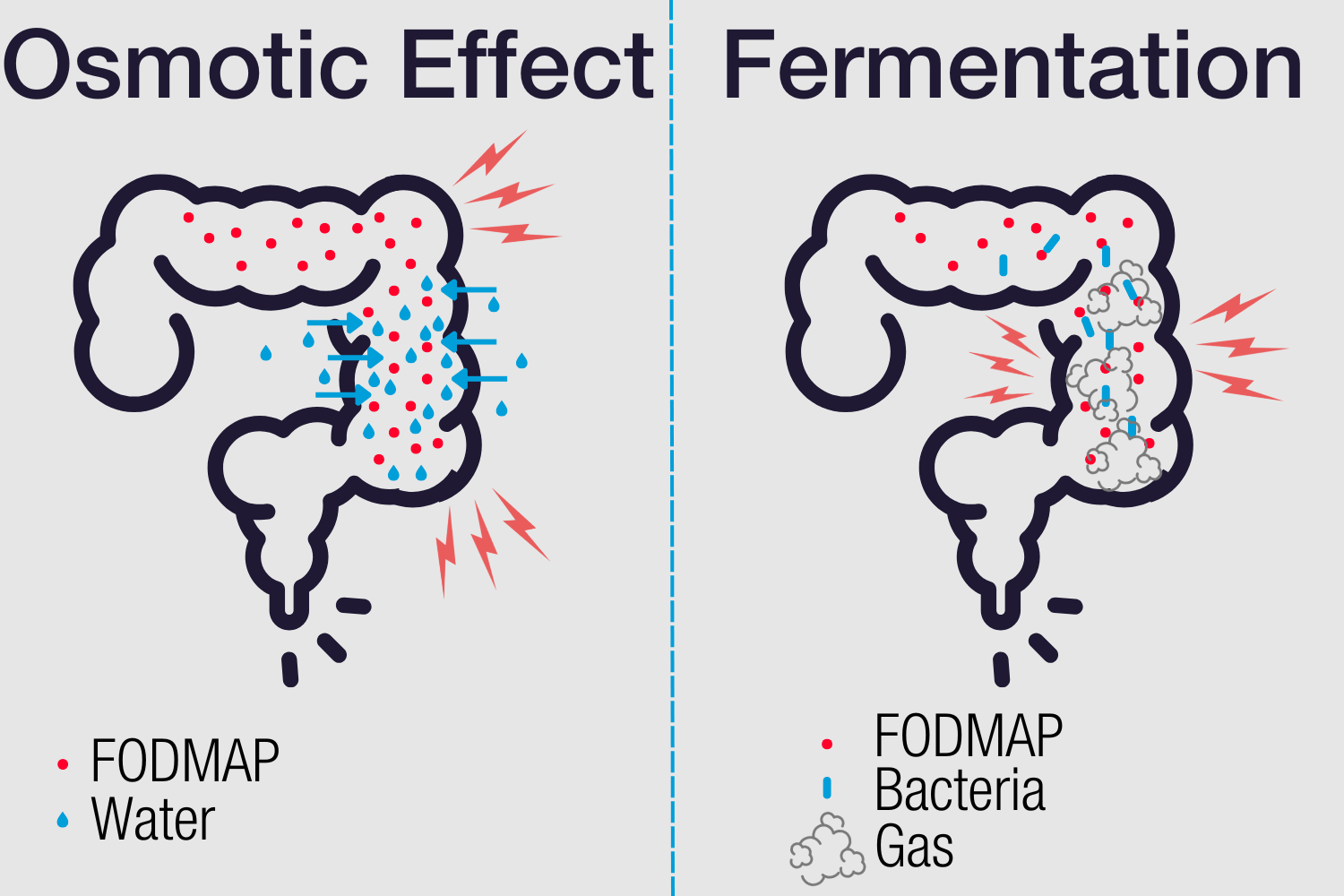
- Osmotic Action: FODMAPs are highly osmotic, meaning they draw massive amounts of water into the bowel. This sudden influx of fluid rapidly alters bowel motility, frequently resulting in acute, watery diarrhea (Bristol Scale Types 6 and 7).
- Bacterial Fermentation: The millions of bacteria residing in the colon begin to rapidly feed on these undigested carbohydrates. The fermentation process produces large volumes of hydrogen and methane gas. This gas rapidly expands the bowel wall, causing severe bloating, visible distension, and agonizing cramping due to visceral hypersensitivity.
The Three-Phase Protocol
Here's what's often misunderstood: the Low-FODMAP diet is a temporary diagnostic tool, not a permanent way of eating. It's designed to calm the gut and identify your specific triggers, and it should be executed in three distinct phases:
Phase 1: Elimination (2 to 6 Weeks)
During this strict phase, all high-FODMAP foods are completely removed from the diet. The goal is to establish a baseline—where symptoms like bloating, pain, and unpredictable bowel habits significantly reduce or disappear entirely.
Phase 2: Reintroduction (6 to 8 Weeks)
Once symptoms have stabilized, individual FODMAP groups are systematically reintroduced one at a time, in increasing portion sizes. For example, you might test Fructans by eating a small amount of garlic on day one, then a larger amount on day two, monitoring closely for any symptom relapse.
Phase 3: Personalization
After testing all groups, you build a personalized, modified diet. Most people find they're only sensitive to one or two specific FODMAP categories—highly reactive to Lactose and Polyols, say, but perfectly fine with Fructans. The goal is to return to the least restrictive diet possible while staying symptom-free.
Dietary Guidelines and Substitutions
High FODMAP (Avoid during Phase 1)
- Dairy: Cow's milk, yogurt, ice cream.
- Grains: Wheat-based bread, pasta, cereals.
- Vegetables: Garlic, onions, asparagus, artichokes, cauliflower.
- Fruits: Apples, cherries, peaches, watermelon.
- Legumes: Beans, lentils, chickpeas.
Low FODMAP (Safe during Phase 1)
- Dairy Alt: Almond milk, lactose-free milk, hard cheeses (cheddar, brie).
- Grains: Oats, quinoa, rice, 100% spelt bread.
- Vegetables: Zucchini, eggplant, potatoes, tomatoes, cucumber.
- Fruits: Blueberries, strawberries, oranges, kiwi.
- Proteins: Eggs, firm tofu, plain chicken, beef, fish.
The Importance of Medical Supervision
Clinical research shows the Low-FODMAP protocol reduces IBS symptoms in up to 86% of patients—but doing it alone is genuinely hard. High-FODMAP foods contain prebiotic fibers that are essential for feeding beneficial gut bacteria. Restricting all FODMAPs permanently is medically dangerous and leads to a severely compromised gut microbiome.
Managing IBS Flare-Ups?
FODMAP sensitivity is one of the primary drivers of Irritable Bowel Syndrome (IBS). Successfully navigating the Reintroduction Phase requires meticulous data collection to find your exact carbohydrate threshold.
Start Your FODMAP Diary NowSources & Medical References: